Conventional Insemination and ICSI
Conventional insemination and intracytoplasmic sperm injection (ICSI) are two insemination methods used during In-vitro Fertilization (IVF) treatment. When IVF was first developed, the eggs were fertilized by sperm naturally in the laboratory by conventional insemination method. Whilst this was very successful in treating couples with infertility due to factors such as tubal blockage, it was not an effective treatment in severe male factor infertility when the sperm failed to fertilize the eggs in the laboratory. ICSI is an assisted fertilization procedure that has been introduced in 1992 to overcome this problem. It involves injection of a single sperm into an egg to help fertilization.
(I) Conventional Insemination
Conventional insemination is a process by which the sperm and eggs are mixed together, and the sperm penetrate the eggs by themselves. This insemination method is suitable for couples with adequate active and normal sperm.
Conventional insemination: the egg is placed with approximately 50,000 to 100,000 active sperm and kept in an incubator.
(II) Intracytoplasmic Sperm Injection (ICSI)
ICSI is a procedure by which an embryologist injects a single sperm into the center of each egg using a micro-injection needle to assist fertilization, thus bypassing any potential problems the sperm will have in getting inside the egg. It is performed for couples with certain indications:
-
One or more of the sperm parameters is/are poor such as low sperm count, poor motility and/or poor morphology (abnormal shape).
-
A previous IVF using conventional insemination had none or very few of the eggs fertilized.
-
The sperm have to be collected surgically from the testicles.
-
The embryos will be tested for a genetic condition (pre-implantation genetic testing or PGT), ICSI will be used to prevent sperm sticking to the outside of the eggs during conventional insemination from interfering with the results.
-
The eggs had been frozen and now are thawed for IVF treatment, the freezing process makes the outer coating of the eggs too tough for sperm to penetrate.
-
The frozen-thawed sperm do not appear especially active, ICSI may be recommended.
Intracytoplasmic sperm injection (ICSI)
ICSI procedure: a single sperm is injected directly into the cytoplasm of an egg.
How does a couple know if they need ICSI?
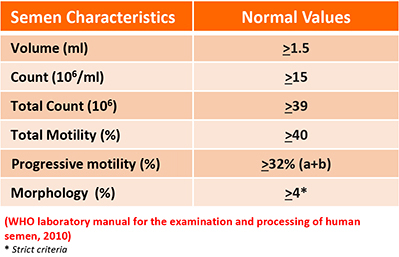
The husband has to undergo a semen analysis before IVF treatment, preferably in our IVF centre so that our embryologists can assess the quality of the sperm in detail, with reference to the WHO laboratory manual for the examination and processing of human semen published in 2010. Based on the results, the doctor will then decide which insemination method is more suitable. The doctor may talk to our embryologists before making a decision. Sometimes, the husband may be asked to give another sample to help them decide. In some circumstances, the sperm quality may fluctuate widely, then the decision may have to be made on the day of egg collection, based on the quality of the sperm on that day.
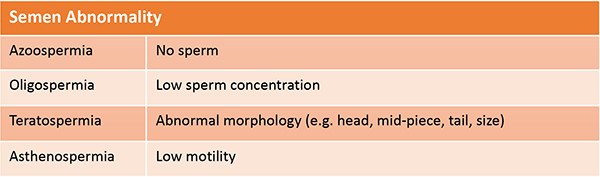
Spermatozoa structure
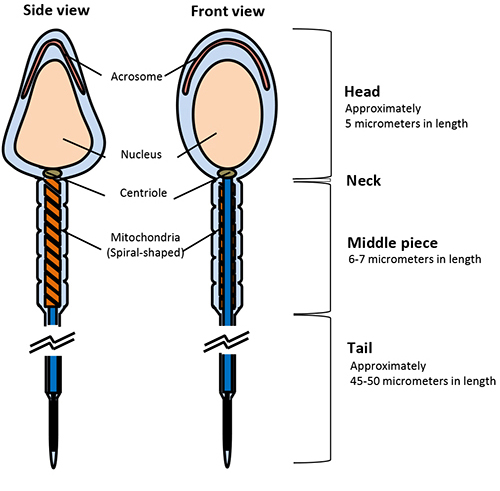
Normal human spermatozoa possess:
-
a smooth oval head shape;
-
acrosome covering 40–70% of the apical part of the head;
-
the head should be broad, with only one tail which is symmetrically attached;
-
behind the head is the mid-piece;
-
the tail is around 45–50 μm in length, it should be not be coiled or bent.
All borderline forms should be classified as abnormal in order to conform to the “strict criteria” for morphological normality.
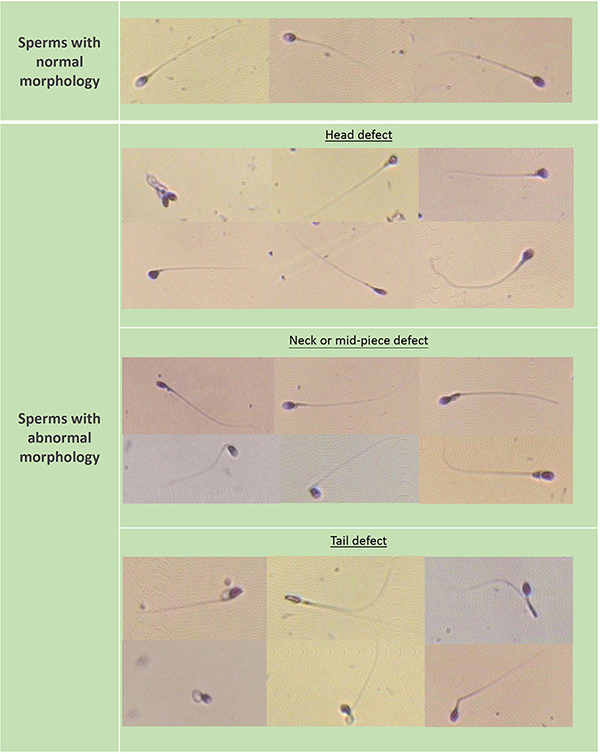
How does a sperm look like?
 scroll right to see more
scroll right to see more
 scroll right to see more
scroll right to see more
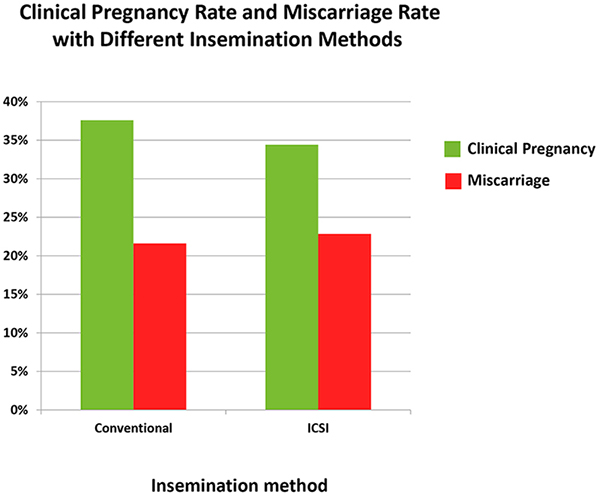
Is it worth having ICSI even if there is no male factor infertility?
For couples who have no evidence of male factor infertility, the chances of getting pregnant are not related to whether they have ICSI or not. Once fertilization happens, the pregnancy rate for a couple using conventional insemination or ICSI is the same.
 scroll right to see more
scroll right to see more